135 results
Removal of Hg(II) from an Aqueous Medium by Adsorption onto Natural and Alkyl-Amine Modified Brazilian Bentonite
- Denis L. Guerra, Emiliano M. Silva, Weber Lara, Adriano C. Batista
-
- Journal:
- Clays and Clay Minerals / Volume 59 / Issue 6 / December 2011
- Published online by Cambridge University Press:
- 01 January 2024, pp. 568-580
-
- Article
- Export citation
-
Mercury ion removal from waste-waters has been the subject of extensive research. The aim of the present investigation was to report the incorporation of the n-alkylamine molecules onto a bentonite surface and the capacities of these new chelating moieties on this modified bentonite surface for mercury removal from water. Bentonite collected from the Amazon region, Brazil, was used in an intercalation process with polar n-alkylamine molecules of general formula H3C(CH2)n-NH2 (n = 1 to 4) in 1,2-dichloroethane. The natural and modified bentonite samples were characterized by elemental analysis, Xray diffraction, helium picnometry, mercury porosimetry, and 29Si, 27Al, and 13C nuclear magnetic resonance spectroscopy. Because of the increasing size of the molecules attached to the pendant chains, the metal-adsorption capability of the final chelating materials was measured in each case. The adsorption of Hg(II) on natural and modified bentonites was determined under different conditions. The effects of concentration of Hg(II), contact time, and pH were investigated; batch and dynamic adsorption experiments of Hg(II) were conducted on bentonite samples under various conditions. The ability of these materials to remove Hg(II) from aqueous solution was assessed by means of a series of adsorption isotherms at room temperature and pH 4.0. In order to evaluate the bentonite samples as adsorbents in a dynamic system, a glass column was filled with clay samples (1.0 g each) and fed with 1.8 × 10−4 mol dm−3 Hg(II) at pH 4.0. The energetic effects caused by adsorption of metal cations were determined by means of calorimetric titrations. Thermodynamics indicated the existence of favorable conditions for such Hg(II)-nitrogen interactions.
ARIPIPRAZOLE-INDUCED OCULOGYRIC CRISIS (ACUTE DYSTONIA)
- L. Rodriguez Andres, C. Vallecillo, L. Gallardo Borge, C. M. Capella Meseguer, G. Guerra Valera, C. Noval Canga
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1009-S1010
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Aripiprazole is a third generation atypical antipsychotic and a dopamine serotonin system stabilizer, effective against positive and negative symptoms of schizophrenia. Within the group of atypical antipsychotics, aripiprazole shows a relatively benign safety profile (e.g. lower metabolic impact, mild effect on cardiovascular parameters), although the reported rate of extrapyramidal side effects is measurable.
Oculogyric crisis (OGC) is a rare movement disorder characterized by a prolongued involuntary upward deviation of the eyes, lasting minutes to hours. In most cases, OCG is a drug-induced adverse event with acute or tardive onset often attributable to a functional impairment of dopaminergic neurotransmission.
ObjectivesOGC is seldom reported in children and young adults during treatment with aripiprazole, althouh it is commonly used in youths.
MethodsWe report a case of an aripiprazole-induced oculogyric crisis in a 19 year old girl who diagnosed with schizophrenia (paranoid).
ResultsThere was a complete remission of the OGC’s following aripiprazole dose reduction, suggesting the clinical manifestation was a dose-dependent phenomenon.
ConclusionsThe present report should raise awarness among clinicians for this relevant possible adverse event, that can happen also with the use of aripiprazol, not only with typical or more antidopaminergic antipsychotics. Future research in the field should emphasize neurobiological dysfunctions as the basis of EPS/OGC in patients.
Disclosure of InterestNone Declared
“Asking for help, quite a challenge”. Time from onset of symptoms to consultation with a psychiatrist
- T. Jiménez Aparicio, M. Fernández Lozano, M. Merizalde Torres, E. Domínguez Guerra, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S469-S470
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the biggest challenges for primary care professionals is to know when it is appropriate to request a consultation with a psychiatrist. A complete medical history should be performed to detect anxious-depressive symptoms, as well as to determine the intensity, the trigger, time of evolution, and the functional repercussion (1). It is also important that the patient is able to express his or her symptoms and ask for help. The concept of “Alexitimia” refers to the difficulty of expressing feelings verbally, and is a frequent symptom in depressive patients (2).
In mild cases and with little repercussion, the physician himself can initiate treatment and follow up (3). However, on other occasions, it will be advisable to request a consultation with psychiatry.
ObjectivesThe main objective is to observe the time that elapses from the onset of symptoms until consultation with the Mental Health team is finally requested. Some preliminary results can already be obtained from this data collection.
MethodsWe have decided to carry out a descriptive study, collecting different variables from patients attending a first Psychiatry consultation.
ResultsIn a total sample of 208 patients, the majority (67%) were between 31 and 60 years old. Following the DSM-V criteria (4), patients were classified into groups according to their disorder: Adaptive, depressive, or other. These data were cross-referenced (Figure 1).
Subsequently, the time elapsed from the onset of symptoms (referred by the patients) was collected, until the referral to Psychiatry was processed. In order to make a comparison, average time (in days) was calculated for the different groups according to their age and diagnosis.
Those patients under 30 years were referred to psychiatry later. A downward trend was seen as the age range increased. In the “younger than 30” and “between 31 and 60” groups, patients who met criteria for Depressive Disorder took longer to be referred, which was striking considering that they are usually considered as more severe patients (Figure 2). This can be attributed to a greater difficulty in expressing their emotions (alexithymia), as another depressive symptom. Disaggregating these data by gender, the patients who clearly took the longest to be referred were men under 30 years old with a final diagnosis of Depressive Disorder (Figure 3). This gender difference is consistent with the social impact of alexithymia according to some articles (5).
Image:
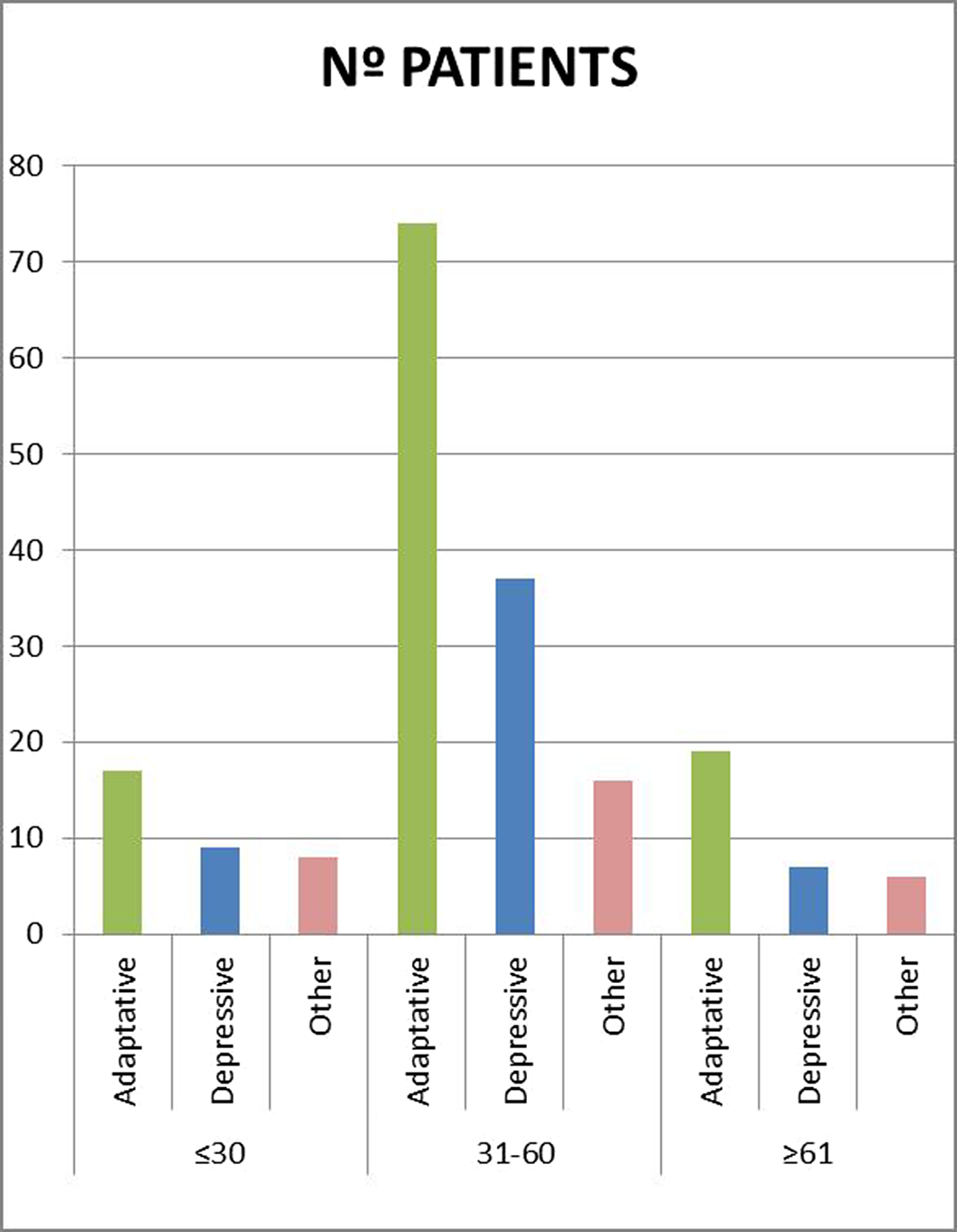
Image 2:
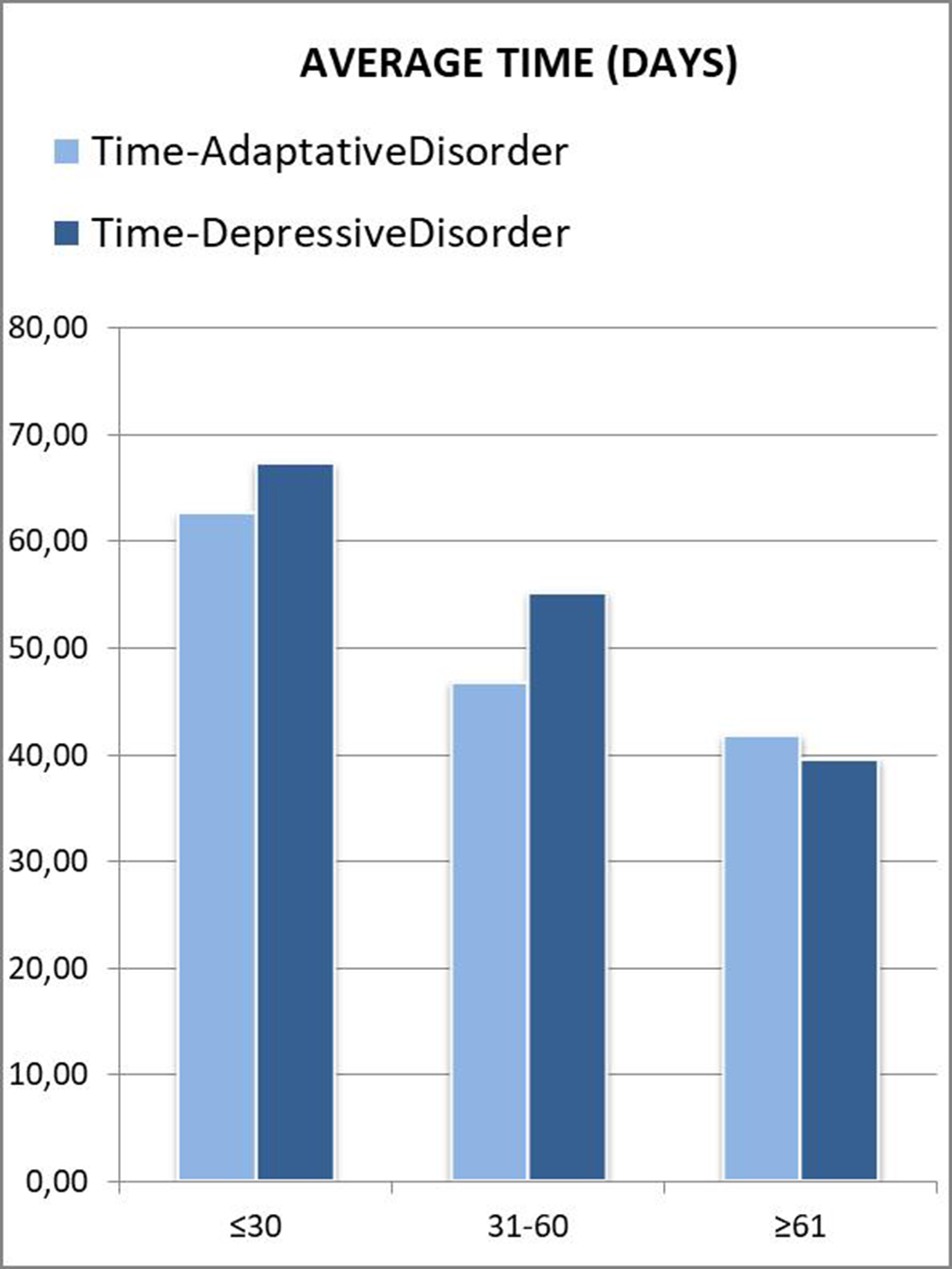
Image 3:
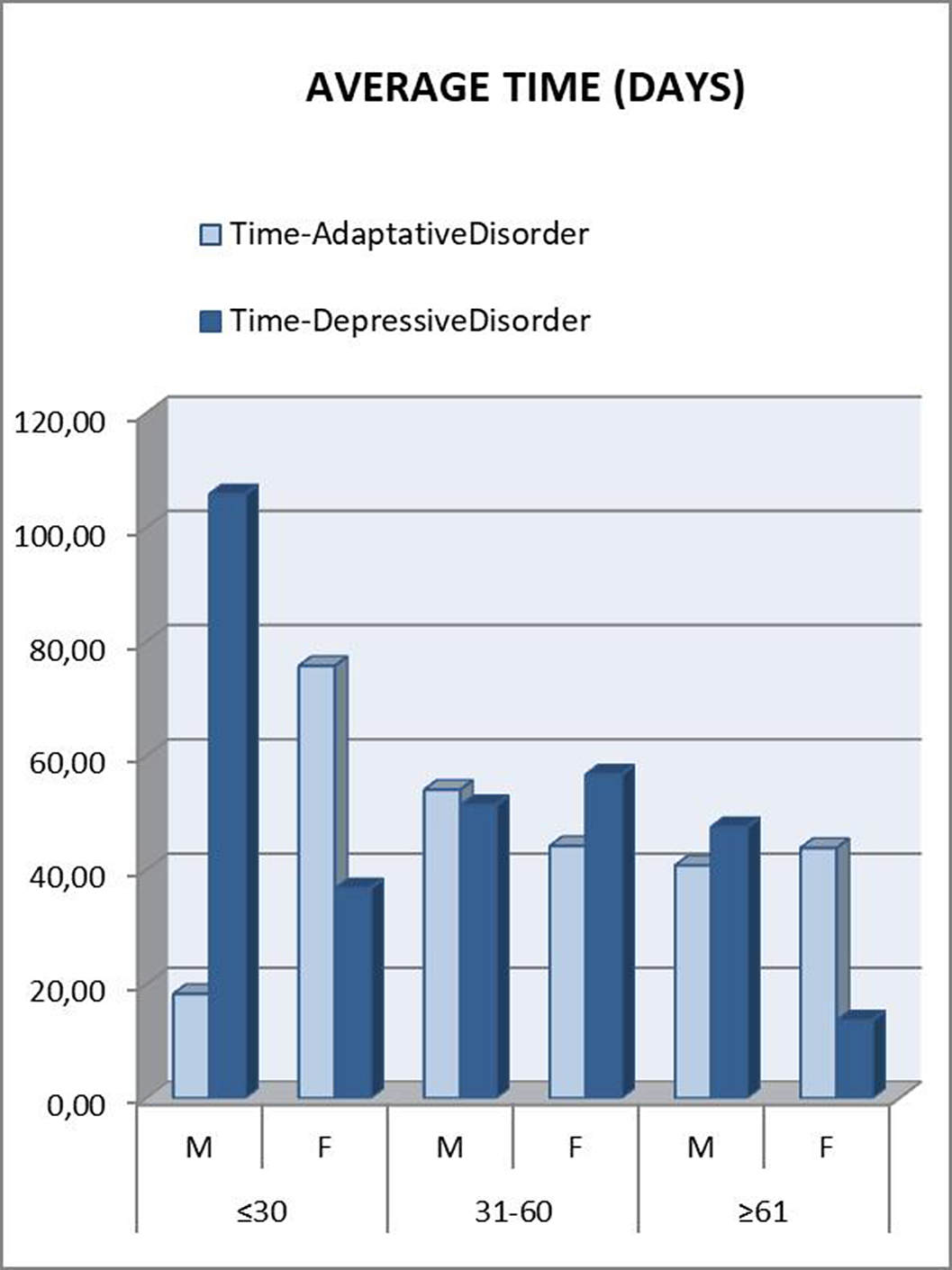 Conclusions
ConclusionsIt is important that primary care physicians know how to take a complete history in those patients with symptoms of anxiety and depression.
In many cases, patients themselves have difficulties expressing their emotions and feelings (alexithymia), which may be another symptom of their discomfort.
This may lead to a delay in the time until referral to a psychiatry is requested, and therefore a worsening of symptoms.
Disclosure of InterestNone Declared
DOCTOR, I’M PREGNANT. Psychopharmacological treatment of depression in pregnant women. A clinical case of a pregnant woman and major depressive disorder
- M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, M. Fernández Lozano, I. D. L. M. Santos Carrasco, N. De Uribe Viloria
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1011
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depression during pregnancy can appear with a prevalence of up to 11% of pregnant women. Psychotherapeutic treatment in these cases is considered the first option, but treatment with antidepressants is sometimes required in these cases.
ObjectivesTo present a clinical case of a pregnant patient diagnosed with depression.
MethodsLiterature review of the psychopharmacological treatment of depression during pregnancy and possible complications.
ResultsA 25y Year old woman, 22 weeks pregnant, who lives with her partner. She has no background in mental health. Paternal aunt diagnosed with type I Bipolar Disorder. She goes to the Mental Health Center for evaluation, due to anxiety and depressive symptoms of 4 weeks of evolution, she refers sadness and apathy, continuous crying, somatic anxiety and obsessive ruminations in relation to childbirth and inability to care for your child. Suicidal ideation as a resolution of her discomfort. She presents with global insomnia and a significant loss of appetite, with a weight loss of 3 kg. Treatment with sertraline 50 mg/day was started, with good tolerance and clinical response
ConclusionsThe psychopharmacological treatment of antenatal depression is a challenge for the psychiatric professional. In all cases, an adequate balance must be made between the risks and complications for the fetus and the psychopathological stability of the pregnant woman. Among the main risks of untreated depression are: preterm delivery and low birth weight, an increased risk of suicide and alterations in the development during the baby’s infancy. The most used antidepressants are the SSRIs, with sertraline being a good option. Paroxetine has been associated with cardiac defects in the newborn. There are studies with tricyclics and duals but no specific teratogenic pattern has been seen. They are associated with an increased risk of spontaneous abortion. Exposure during the third trimester may be associated with obstetric complications.
Disclosure of InterestNone Declared
Late-onset schizophrenia: a differential diagnosis
- M. V. López Rodrigo, M. Palomo Monge, A. Osca Oliver, F. Tascón Guerra, V. Ros Fons
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1071-S1072
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Regarding the diagnosis of schizophrenia, a peak of onset of symptoms is considered at 25 years. The debut after 60 years is considered late onset and is rare, generating controversies in the diagnosis
ObjectivesWe present the case of a 58-year-old patient with no personal or family history of mental health, who came to the emergency room for the first time, reporting feeling in danger. He comments itching on his skin, verbalizing seeing bugs running through it, relating this phenomenon to “witchcraft by my brothers”, he also refers to feeling like “they watch my thoughts and block it through a mobile application, they enter through my eye right and this gives me less vision and a headache. He also refers to having the ability to listen to how his brothers talk about how they are going to “hurt me.” Psychopathologically, we highlight that she is oriented in the three spheres, presenting delusional ideation with an experience of harm, a phenomenon of thought theft and auditory and tactile hallucinations.
MethodsAnalytical and imaging tests, as well as toxins in urine, were negative.
ResultsDiagnosis of psychotic episode is made to see evolution. The clinic partially yields to treatment with atypical antipsychotics. At this time, the patient has no awareness of the disease.
ConclusionsDespite being a diagnosis that is scarcely prevalent, once organic disease has been ruled out.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Postictal psychosis in a psychiatric pacient, about a case
- M. V. López Rodrigo, M. Palomo Monge, A. Osca Oliver, V. Ros Fons, F. Tascón Guerra
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S616
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Postictal psychosis is the most frequent psychosis in epileptic patients, appearing between 3-8% of them. As temporary criteria, it must appear in less than a week after the epileptic crisis, with a duration of between 15 hours and 3 months.
ObjectivesWe present the case of an 82-year-old patient admitted to the ED due to an epileptic seizure. Request evaluation for agitation and disorientation.
MethodsThis is an 82-year-old patient diagnosed with epilepsy for 5 years, with unwitnessed seizures, under treatment with levetirazetam. In the last consultation with neurology, the differential diagnosis was raised with anxiety crises due to normal intercritical EEG.The patient went to the emergency room after a partial crisis, presenting a post-critical state and beginning hours later with disorientation in time and place, manifesting delusions of religious content, as well as visual hallucinations of the same type, presenting agitation that required pharmacological and mechanical restraint.
ResultsAdmission to the Neurology Service was decided, with a good response to treatment with a typical intramuscular antipsychotic, with complete remission of the condition in 48 hours. Small areas of ischemia compatible with the patient’s age are observed in the cranial CT and the EEG shows slowed global activity.
ConclusionsPostictal psychosis is a phenomenon of low prevalence, however, it is important to take it into account. It is important to recognize the postictal “lucid” period in patients with a family or personal history of psychiatric illness and seizures with compromised consciousness.
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
Bipolar disorder and substance use: Risk factors and prognosis
- M. Fernández Lozano, B. Rodríguez Rodríguez, M. J. Mateos Sexmero, N. Navarro Barriga, C. Vallecillo Adame, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. P. Pando Fernández, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder comorbidity rates are the highest among the major mental disorders. In addition to other intoxicants, alcohol is the most abused substance because it is socially accepted and can be legally bought and consumed. Estimates are between 40-70% with male predominance, which further influences the severity with a more complicated course of both disorders.
ObjectivesThe objective of this article is to highlight the impact of substance use on the course and prognosis of bipolar disorder, as well as to make a differential diagnosis of a manic episode in this context.
MethodsBibliographic review of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 45-year-old male patient. Single with no children. Unemployed. History of drug use since he was young: alcohol, cannabis and amphetamines. Diagnosed with bipolar disorder in 2012 after a manic episode that required hospital admission. During his evolution he presented two depressive episodes that required psychopharmacological treatment and follow-up by his psychiatrist of reference. Since then, he has been consuming alcohol and amphetamines occasionally, with a gradual increase until it became daily in the last month. He went to the emergency department for psychomotor agitation after being found in the street. He reported feeling threatened by a racial group presenting accelerated speech, insomnia and increased activity.
ConclusionsThe presence of substance abuse complicates the clinical presentation, treatment and development of bipolar disorder. It is associated with a worse prognosis with multiple negative consequences including worsening symptom severity, increased risk of suicide and hospitalization, increased medical morbidity and complication of social problems. In addition, this comorbidity delays both the diagnosis and treatment, by masking the symptoms, and making more difficult an adequate differential diagnosis.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
PEAKS AND VALLEYS: BIPOLAR DISORDER, RAPID CYCLERS AND ENERGY DRINKS CONSUMPTION
- M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martinez Gimeno, P. Pando Fernández, B. Rodriguez Rodriguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. D. C. Vallecillo Adame, T. Jimenez Aparicio, C. de Andres Lobo, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S702-S703
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar Disorder (BD) is considered a serious mental disorder characterized by a changing mood that fluctuates between two completely opposite poles. It causes pathological and recurrent mood swings, alternating periods of exaltation and grandiosity with periods of depression. We talk about rapid cyclers when four or more manic, hypomanic or depressive episodes have occurred within a twelve-month period. Mood swings can appear rapidly. Approximately half of the people with bipolar disorder may develop rapid cycling at some point.
ObjectivesPresentation of a clinical case about a patient with Bipolar Disorder with rapid cycling and poor response to treatment.
MethodsReview of the scientific literature based on a clinical case.
Results33-year-old male, single, living with his mother, under follow-up by mental health team since 2012. First debut of manic episode in 2010. The patient has filed multiple decompensations related to consumption of toxics (alcohol and cannabis). Currently unemployed. He attended to the emergency service in June 2022 accompanied by his mother, who reported that he was restless. The patient refers that he has interrupted the treatment during the vacations, having sleep rhythm disorder with abuse of caffeine drinks. Currently the patient does not recognize any consumption.The patient reports that during the village festivals he felt very energetic, occasionally consuming drinks rich in taurine and sugars, even having conflicts with people of the village. Finally, the patient was stabilized with Lithium 400 mg and Olanzapine. In September, the patient returned to the emergency service on the recommendation of his referral psychiatrist due to therapeutic failure. The only relevant finding we observed in the analytical determinations were low lithium levels (0.4 mEq/L). The transgression of sleep rhythms and the abuse of psychoactive substances required the admission of the patient to optimize the treatment (Clozapine, Lithium, Valproic Acid). At discharge, he is euthymic, has not presented behavioral alterations and is resting well. Finally, it was decided that the patient should go to the Convalescent Center to continue treatment and achieve psychopathological stability.
ConclusionsBipolar disorder is an important mental illness, having an incidence of 1.2%, being responsible for 20% of all mood disorders. Therefore, it is important to perform an adequate and individualized follow-up of each patient. Treatment with mood stabilizers tries to improve and prevent manic and depressive episodes, improving chronicity and trying to make the long-term evolution as good as possible, being important psychoeducation and psychotherapy.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
Memory complaints and quality of life in a patient with mild cognitive impairment
- M. P. Pando Fernández, M. A. Andro Vidal, M. Calvo Valcarcel, P. Martinez Gimeno, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, C. De Andrés Lobo, T. Jimenez Aparicio, C. Vilella Martin, M. Fernández Lozano, B. Rodríguez Rodríguez, M. J. Mateos Sexmero, N. Navarro Barriga
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S937-S938
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Subjective memory complaints remain a relevant aspect to be considered in patients with mild cognitive impairment. Likewise, their association with depressive symptoms, quality of life and cognitive performance is also an objective to be studied in such patients.
ObjectivesOur clinical case represents just one opportunity to study how memory complaints are related to depressive states and how they affect the quality of life of patients with mild cognitive impairment.
MethodsWe conducted a bibliographical review by searching for articles in Pubmed.
ResultsPERSONAL HISTORY: Male, 73 years old, separated, residing alone in Valladolid. He has home help, a person comes to help him with the household chores. Little social and family circle.
History in Mental HealthHe has a history of an admission in 2013 to this Short Hospitalization Unit for ethanol detoxification. Since then, he has been followed up in the Mental Health Unit. According to the reports, he has been diagnosed with depressive disorder and cluster B personality disorder.
Current psychopharmacological treatment: diazepam, olanzapine, duloxetine 60 mg, quetiapine.
Toxic habits: history of chronic ethanol consumption. Smoker. He denies other toxic habits.
Current EpisodeThe patient presents a worsening of his mood of 15 days of evolution, coinciding with a voluntary decrease of his psychopharmacological treatment that the patient has carried out on his own. He walks with the aid of a crutch. Hypomimic facies. Slowed language, circumstantial, with speech focused on current discomfort.
On assessment, he reports initial improvement after reducing his medication, but in recent days he has experienced a decrease in initiative accompanied by feelings of emptiness, sadness and loneliness. He refers to memory complaints for which he is awaiting evaluation by Neurology. The patient explains that at other times in his life he has presented self-harming ideas that he has been controlling. At this time he expresses desire for improvement and adequate future plans, and accepts plans to attend a memory workshop. He also reports visual hallucinations with no affective repercussions and preserved judgment of reality.
Therapeutic PlanTreatment adjustment: Duloxetine 60 mg, 2cp/day. The patient is recommended to lead an active lifestyle and attend a day center or memory workshop.
ConclusionsIn numerous patients with mild cognitive impairment, we have observed that memory complaints are closely related to depressive symptoms and to the patient’s functioning in daily life.
In one study memory complaints were a negative predictor of quality of life in these patients.
Therefore, in addition to considering the importance of treating depressive symptoms, it is also important to address quality of life in patients with mild cognitive impairment.
Disclosure of InterestNone Declared
Specific treatment for alcohol use disorder reduces relapse after psichiatric hospitalization
- O. Martin-Santiago, J. I. Goncalves-Cerejeira, G. Guerra-Valera, M. Calvo-Valcarcel, P. Martinez-Gimeno
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S565
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients with an alcohol use disorder frequently relapse after various efforts to quit. Admission to hospital units is a possible start to stop drinking alcohol and reach abstinence. Among the pharmacological strategies to quit this addiction are specific drugs, such as disulfiram or namelfen, which are widely studied. Hospitalized patients frequently initiate these medications to control addiction, but little is known about their efficacy after discharge in this group.
ObjectivesThe aim is to determine whether the initiation of treatment with specific drugs for alcohol use disorder could help to maintain alcohol abstinence after admission to a General Hospital Psychiatric Ward. In addition, we want to check those factors associated with a higher rate of relapse in consumption.
MethodsWe conducted a retrospective cross-sectional study of a group of patients admitted in 2018 to a psychiatric hospitalization ward due to alcohol use disorder and who expressed their desire to stop drinking. At the time of admission, we recorded sociodemographic data, consumption of other substances and alcohol family history. Patients initialized specific treatments to reduce and control alcohol consumption if they wanted. Twenty-four months after discharge, we acquired the number of relapses through new admissions, emergency room visits or outpatient follow-up data.
ResultsA sample of 36 patients (28 men) admitted to a psychiatric hospitalization ward was analyzed. At discharge, 17 accepted specific pharmacological treatments to reduce alcohol consumption. After a follow-up period of 24 months, 70.8% relapsed compared to 94.7% who did not accept treatment (χ2=4.001, DF=1, p=0.045, OR=0.13). There were no differences between the two groups in age, gender, amount of alcohol consumed, follow-up modality at discharge or if it was their first detoxification attempt. However, those who did not accept the specific pharmacological treatment consumed other drugs (41.1% vs 5.8%, χ2= 5.888, DF=1, p=0.015), had other history of mental disorder (64.7% vs 23.5%, χ2= 5.845, FD=1, p=0.015) and a higher proportion of relatives with alcohol consumption (81.8% vs 42.8%, χ2= 3.896, FD=1, p=0.048) more frequently. The time (in days) to relapse was faster in this group of patients (200.8 vs 402.7 , Z=-2.5413, p=0.005).
ConclusionsAccepting drug-specific treatment for alcohol use can be helpful for many patients who want to achieve alcohol abstinence. Among the factors that prevent the acceptance of this treatment is the consumption of other substances, comorbidity with another mental pathology and family history, which may involve genetic factors that favour addiction. This group of patients could benefit from a specific pharmacological treatment, although other psychosocial factors may also help.
Disclosure of InterestNone Declared
Delusional disorder during pregnancy. A case report.
- M. Palomo Monge, M. V. Lopez Rodrigo, C. Garcia Montero, M. F. Tascon Guerra, A. Osca Oliver, A. Duque Dominguez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1070-S1071
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 34-year-old female patient, 35 weeks pregnant and previously diagnosed with delusional disorder.
ObjectivesSomatic personal history: NAMC. intrinsic asthma. Cutaneous psoriasis.
Personal psychiatric history: In psychiatric follow-up since childhood, due to eating problems. Subsequently by adaptive pictures, with anxiety and dysfunctional personality traits intermittently. She resumes contact again in February 2017 presenting frank delusional clinic. Father diagnosed with schizophrenia.
Personal data: 34-year-old woman, married, with a 6-year-old son.
MethodsCurrent illness: The patient presents active delusional symptoms of about 3 years of evolution, she reports that she knows that there are people in her neighborhood who want to harm her and have guns with which they are constantly shooting to kill her "I hear the shots every day, I have the windows covered with metal plates and I cannot go out with my son, nor to the park, nor to do the shopping”. When she began the delusional symptoms, she was prescribed treatment with olanzapine without response, later with paliperidone palmitate, without response, and then with oral aripiprazole and depot 400mg once a month, with partial response. Prior to the current pregnancy, treatment with clozapine was considered, which the patient accepted but did not tolerate and had to be withdrawn.
ResultsEvolution: The patient then remains in treatment with depot aripiprazole, with a partial response and less behavioral repercussion of the delusional content, but with a torpid evolution and tending to chronicity. During this course the patient accidentally becomes pregnant again. The doses of benzodiazepines that she was previously taking to control anxiety and sleep were lowered, maintaining treatment with depot aripiprazole, reducing the dose to 300mg monthly. The pregnancy has proceeded normally to date, with close controls by the gynecology service and monthly visits to psychiatry clinics.
ConclusionsClinical judgment: Persistent delusional disorder.
In this case, the need arises to maintain depot antipsychotic treatment in a patient with a severe mental disorder during pregnancy, given the serious consequences of delusional content on the patient’s functioning and thus be able to preserve stability at this level during pregnancy.
Disclosure of InterestNone Declared
“We weren’t used to seeing our colleagues hospitalized”: A clinical-qualitative study on reports from an intensivist clinical team at a Brazilian university public hospital
- E. R. Turato, F. S. Santos, L. M. Guerra, A.-P. D.-C. Gasparotto, R. N. Aoki, J. M. Cavalcante
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S787
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The care relationships of physicians and nurses with patients with Covid-19 had pointed to a scenario explorable from a psychological point of view due to the peculiarities of this pandemic. How do clinicians feel, when caring for their co-workers, in a context that was not so common to see colleagues occupy the patient’s place? What emotional experiences arise from this reality? The results of the present study sought to point out how to handle this caring relationship, in an exceptional context.
ObjectivesTo interpret emotional meanings reported by physicians and nurses on their experiences of working at COVID-19 intensive care units during the height of the pandemic.
MethodsClinical-qualitative design of Turato. Data collection with semi-directed interviews with open-ended questions in-depth applied to a sample of six professionals, closed by theoretical information saturation according to Fontanella, in a Brazilian university general hospital. Trigger question: “Talk about the psychological meanings of your experience in face of management of patients with COVID-19 at ICU”. Data treatment by the Seven Steps of the Clinical-Qualitative Content Analysis of Faria-Schützer. Theoretical framework from Medical Psychology using Balintian concepts.
ResultsWe raised initially 4 categories. Three categories were presented preliminarily in this congress, version last year. In this opportunity, we show this special category of analysis that emerged during the deepened discussion of the final results: “The feeling of insecurity: from technique to affective dimension”.
ConclusionsThe care relationships between the health professional and the patient hospitalized in the Covid-19 ICU pointed to peculiar transference and countertransference psychodynamic mechanisms between both. Before the pandemic, the care relationship seemed pragmatic and protocolar. During the pandemic, this relationship seemed “more subjective”, building a strongly emotional dimension, as health professionals also began to care for their colleagues in the profession. The egoic defense mechanisms, such as projective and introjective identification were reported as intense.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
“Keeping an eye on amylase”. Side effects of antidepressants
- T. Jiménez Aparicio, G. Medina Ojeda, A. Rodríguez Campos, L. Rodríguez Andrés, C. Vallecillo Adame, C. De Andrés Lobo, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. J. Mateos Sexmero, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M. P. Pando Fernández, P. Martínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Both in consultations with the general practitioner and with the psychiatrist, antidepressants are one of the most used drugs (1). These have multiple indications, and there are different groups according to their mechanism of action. In relation to this case, we are going to talk about Venlafaxine, a dual-type antidepressant, that is, it inhibits the reuptake of serotonin and norepinephrine. One of the most common side effects is digestive discomfort, which usually resolves after a few weeks (2). However, we should not ignore these symptoms, since they can hide something more serious.
ObjectivesPresentation of a clinical case on a patient who presented an increase in pancreatic amylase after starting treatment with Venlafaxine.
MethodsBibliographic review including the latest articles in Pubmed on side effects of antidepressant treatment, and more specifically at the gastrointestinal level (in this case we will talk about pancreatitis).
ResultsWe present the case of a 49-year-old woman, who was hospitalized 2 years ago, due to a first depressive episode. During this admission, psychopharmacological treatment was started for the first time, on that occasion with a selective serotonin reuptake inhibitor (SSRI), treatment of first choice (3). The patient had no side effects at that time, but the response was very modest, so it was decided to replace that antidepressant with Venlafaxine (with dual action), up to 150mg. The depressive symptoms improved markedly, however the patient began to feel digestive discomfort (which at first did not seem to be of great importance). A general analysis was performed, in which an increase in lipase (978 U/L) and amylase (528 U/L) was detected. An echoendoscopy, an abdominal scan, and a magnetic resonance cholangiography were performed; Pancreatitis secondary to drugs was suspected (a severe condition). Luckily, no significant lesions were found in the tests, and the levels of amylase and lipase decreased when Venlafaxine treatment was withdrawn (without reaching the normal range). The patient was discharged and continued to attend consultations. In the last control, amylase had dropped to 225 U/L. His abdominal pain disappeared. Treatment with Vortioxetine (a multimodal antidepressant) was started, however the amylase levels continue to be monitored, and the patient continues to see the gastroenterologist.
ConclusionsGastrointestinal side effects are very common when taking antidepressant treatment, and in most cases they do not usually represent a serious problem.
However, it is described in the scientific literature that in some cases, acute pancreatitis secondary to some drugs, including Venlafaxine, can occur (4). In order to detect it, it is necessary to perform a blood test and sometimes also other complementary tests.
For its treatment, the fundamental thing is to withdraw the causing drug, trying to find other alternatives, and carry out a control to monitor possible complications
Disclosure of InterestNone Declared
My stomach is full
- M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, N. De Uribe Viloria, G. Guerra Valera, T. Jiménez Aparicio, C. Vallecillo Adame, C. De Andrés Lobo, I. Santos Carrasco, J. Gonçalves Cerejeira, N. Navarro Barriga, M.J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S583
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is an eating behavior disorder that is often related to various personality factors. The relationship between obsessive compulsive disorder and eating Disorders has been highlighted.
ObjectivesTo present a clinical case of a patient with eating disorder and gastric bezoar, secondary to compulsive hair ingestion.
MethodsBibliographic review of articles published in relation to the comorbidity of these disorders, based on articles published in the last 5 years in Pubmed.
Results26-year-old female. Diagnosis of restrictive anorexia nervosa. She was admitted to the hospital on two occasions for nutritional disorders. In the last admission, she reported greater anxiety and significant weight loss. She reports that she has limited her food intake, but she does feel thin and is unable to eat for fear of gaining weight. Ruminative thoughts about her body image. During admission, the patient expressed a sensation of fullness, nausea and vomiting, later observing in abdominal X-ray and gastroscopy, the presence of a gastric trichobezoar, which was finally resolved conservatively.
ConclusionsTrichotillomania is observerd in 1 in 2000 people, trichophagia is even less frequent. According to DSM- V, these disorders are grouped within obsessive-compulsive spectrum disorders. A Trichobezoar is a conglomerate that can be found in the stomach or intestine, composed mainly of hair, previously ingested. Trichotillomania can be associated with anorexia nervosa, especially in patients with obsessive personality traits, which occurs frequently. The gastric slowing that patients with anorexia often present is a factor that favors the formation of the bezoar
DisclosureNo significant relationships.







